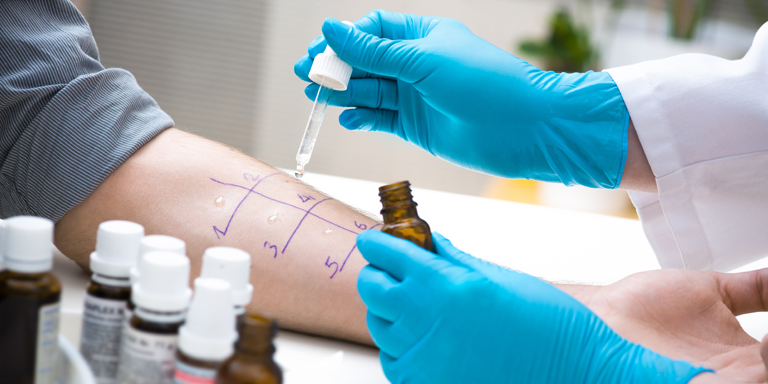
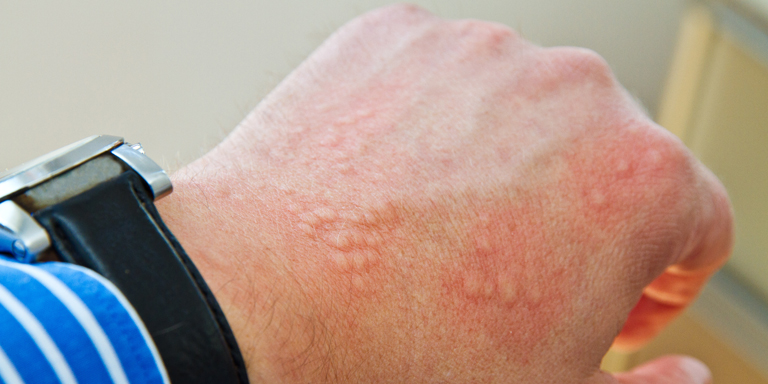
Angioedema
Severe local swelling of the skin might indicate a case of angioedema. The condition mainly affects the arms and legs but can also affect the face and the genital area.
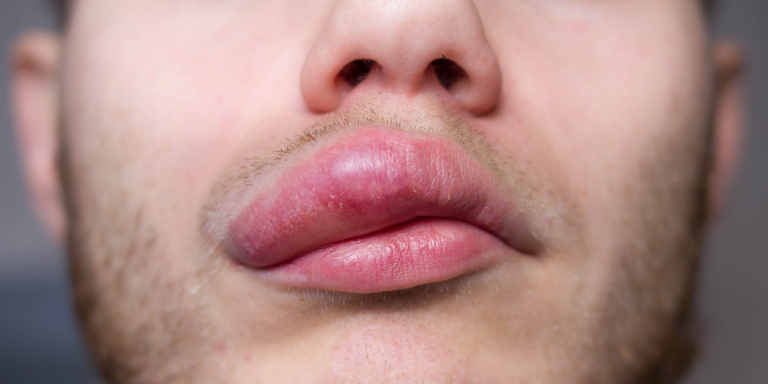
Table of contents:
Our skin is made up of three layers: epidermis, dermis and hypodermis (or subcutaneous layer). Angioedema – also known as Quincke’s oedema or angioneurotic oedema – means accumulations of fluid in the subcutaneous tissue that lead to swelling. Two basic forms of angioedema can be distinguished: Mast cell-mediated or more rarely bradykinin-mediated angioedema.
Causes and forms
Mast cell-mediated angioedema
Most cases of angioedema that occur spontaneously are mast-cell-mediated (also known as mast cell mediator mediated). Mast cells are defence cells of the immune system and are found under the skin, in mucous membranes, near blood and lymph vessels and in the organs. They secrete messenger substances that strengthen the body's immune response. One of these messenger substances is histamine, which increases vessel permeability. With this increase in permeability, blood plasma enters the tissue, resulting in accumulations of fluid. These manifest as swellings under the skin (angioedema) or as wheals on the skin surface (urticaria). Mast cells may be activated by allergic reactions, viral and bacterial infection, medication and even stress.
Bradykinin-mediated angioedema
Bradykinin is a tissue hormone that increases vessel permeability. C1-inhibitor normally regulates the formation of bradykinin. If C1-inhibitor is not available in sufficient quantities, is deficient or too much is consumed, the result is an excess of bradykinin. This also happens when medication blocks the degradation of bradykinin. Due to this excess, more fluid passes from the blood vessels into the surrounding tissues, resulting in angioedema.
Subforms of this group are:
- hereditary angioedema (HAE): Due to a genetic mutation there is a deficiency of C1-inhibitor or it is produced in insufficient quantities (HAE Type 1). Or C1-inhibitor has a reduced function (HAE Type 2). Typical triggers of angioedema attacks include stress, physical exertion, injury, surgery and hormonal changes.
- acquired angioedema: This form is quite rare and is triggered in most cases by autoimmune disease or associated with malignancies.
- drug-induced angioedema: This is caused by certain blood pressure-lowering drugs, especially ACE-inhibitors, and immunosuppressants such as mTOR inhibitors.
- Idiopathic angioedema: This means that there is no known cause for this form of angioedema.
Symptoms
In most cases, angioedema occurs irregularly and with considerable variation in frequency, from once every few years to daily. In both forms of angioedema, the swellings are often combined with a feeling of pressure or a burning sensation, which can at times also be painful. The parts of the body typically affected include:
- head: swelling of the eyelids, lips, facial skin, headaches, dizziness
- mucous membranes of the mouth, in the neck: swelling of the tongue, larynx, starting with a change in voice, hoarseness, shortness of breath
- genital organs: swelling of the penis, testicles, vulva and vagina
- extremities: swellings on hands, feet, arms and legs; normal sequences of movement are restricted, walking impeded.
In mast cell-mediated angioedema, itchy hives (urticaria) may appear on the body at the same time. This is not the case in the bradykinin-mediated form. However, in most cases the swellings are painful.
In hereditary angioedema (HAE), swellings frequently occur in the gastrointestinal tract (especially in the small and large bowel), which can result in abdominal pain, nausea, vomiting and diarrhoea, even lasting several days. Swellings may also occur in the airways and can be very dangerous. Nowadays, however, due to the availability of effective medication, life-threatening situations can be averted in most cases.
Diagnosis
If the swelling is visible, the clinical diagnosis is relatively straightforward. Finding the cause, on the other hand, is often a challenge, which is why it is important for the doctor to question the individual thoroughly when investigating the symptoms. Specific laboratory tests, e.g. to measure the C1-inhibitor level and other parameters, can also aid clarification.
A symptom diary kept by the sufferer can also help identify the cause. In this diary, the sufferer should write down when and how long the swelling occurred and what other symptoms were also present, (such as pain, itching, rash, shortness of breath and abdominal pain). Photographs of the swellings are also very helpful to establish the diagnosis.
Treatment
Mast cell-mediated angioedema
If an allergy is the cause of the angioedema, every effort should be made to avoid the trigger in future. If a bacterial infection or some other illness is the cause, this should be treated appropriately.
In most cases – irrespective of the cause – antihistamine and cortisone are used to alleviate the symptoms of mast cell-mediated angioedema. They are also used as emergency medication in life-threatening situations, where necessary, even in combination with a prefilled adrenaline syringe.
Bradykinin-mediated angioedema
In hereditary angioedema (HAE), the primary aim should also be to avoid the triggers. There is also the option of preventive therapy with certain drugs. C1-Inhibitor and the active substance icatibant – a bradykinin receptor antagonist – can be used to treat an acute attack of angioedema.
It is important for sufferers to have an action plan in place. This helps decide what action to take in any given situation. It is important that family members, friends and, where possible, work colleagues also know about the disease and the action to be taken in emergencies. Furthermore, sufferers should always have an emergency ID card with them. This is issued by the treating doctor. Care is usually provided by the doctor in collaboration with a specialist HAE centre. The Swiss HAE Association can provide further support: www.hae-vereinigung.ch (in German and French)
In acquired angioedema, it is important to ensure that the underlying cause is treated The same medication is effective in emergencies as in hereditary angioedema.
In drug-induced angioedema, administration of C1-inhibitor-Präparaten or icatibant is also useful. The drugs that cause the angioedema should be discontinued and replaced where necessary with medication from a different class of active substance.
Tips and tricks
- If angioedema is suspected, it is best to first consult your doctor. Your doctor may then decide to refer you to a large hospital with an angioedema clinic.
- Drug-induced angioedema can occur for the first time even after prolonged use of the drug (weeks or months). Consult a doctor immediately if the relevant symptoms appear.
- Hereditäry angioedema (HAE) runs in families. Family members should therefore also be tested when a case of HAE is confirmed.
Facts and figures
- Up to 20% of the population are affected by an acute swelling at some point in their lives.
- Angioedema can occur in one or more parts of the body.
Editors: aha! Swiss Allergy Centre in co-operation with the Scientific Advisory Board.