Psoriasis
Psoriasis is a chronic, non-contagious disease that primarily affects the skin.
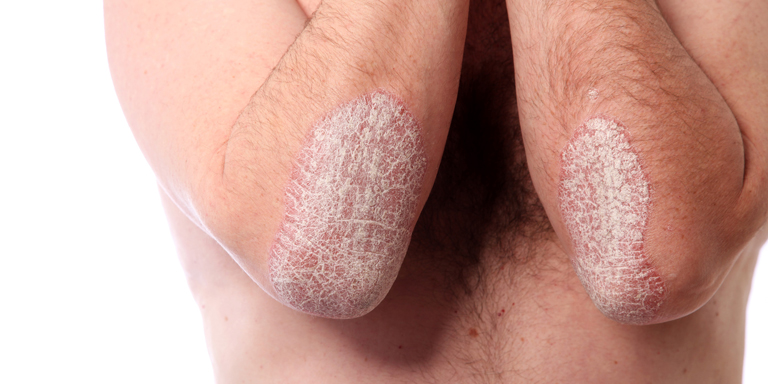
Table of contents:
Psoriasis is one of the most common and widespread diseases of the skin, affecting about 2% of the global population.
Causes and forms
Although psoriasis is non-hereditary, people may be genetically predisposed to its development. However, this does not necessarily mean that they will actually suffer from the disease. How exactly psoriasis develops is still unclear. It is assumed that a number of different factors may play a role and for this reason it is commonly referred to as a multifactorial disease. A combination of a genetic predisposition and environmental factors may cause or aggravate the disease.
Possible triggers include:
- infections
- medication
- metabolic disorders
- hormonal factors
- mental factors
- environmental factors
- injury (e.g. sunburn or cuts and bites)
- pressure points / mechanical irritation
- stress
- alcohol
- smoking
- obesity
Plaque psoriasis (psoriasis vulgaris)
In the most common type of psoriasis, silvery red patches may appear anywhere on the body. These patches or plaques give this type its name – plaque psoriasis. Some patients may also have psoriasis of the finger and toenails (nail psoriasis), with pitting (small pinprick holes) on the nail surface, discolouration (oil spots) and lifting of the nailbed.
Guttate psoriasis
This type of psoriasis is often very itchy and commonly occurs after a bacterial infection. It is characterised by multiple, small psoriatic lesions (guttate means dot-like).
Pustular psoriasis
In this rare and unusual type of psoriasis, pus-filled blisters form on reddened areas of skin. They may form on discrete parts of the body (such as the palms of the hand and soles of the feet) or cover the entire body.
Nail psoriasis
Nail changes may occur in all types of psoriasis. In roughly half of all cases, these changes occur in the fingernails, in slightly fewer in the toenails
Symptoms
95% of psoriasis sufferers have the classic symptoms of psoriasis (psoriasis vulgaris or plaque psoriasis). The disease is characterised by round or oval scaly, red patches of skin. These may appear on any part of the body, but most commonly occur on the scalp, the elbows, the extensor surfaces of the knees, around the cruciate ligaments and in the buttock crease.
These patches develop when the outer skin layer is regenerated too quickly. In healthy skin, this process takes 28 days but the cells in these patches are regenerated in just 8 days. The incomplete keratinisation process leads to the development of silvery patches. The affected areas of skin dry out and the skin may crack or bleed.
In most cases, the disease periodically flares up and subsides. Sufferers may experience severe itching during flare-ups.
About 20% of sufferers also suffer from psoriatic arthritis, a painful inflammation of the joints, tendons and spine that restricts movement.
Diagnosis
Diagnosis is based on the typical symptoms listed above. This requires detailed discussion between the doctor and the sufferer. In some cases, the doctor may also arrange for analysis of a tissue sample (biopsy) to confirm the diagnosis.
Treatment
There is as yet no cure for psoriasis. However, appropriate treatment to alleviate the symptoms can help sufferers largely lead a normal life.
Finding the appropriate treatment is not always easy. What works with one sufferer does not necessarily work with others.
The choice of treatment depends on the following factors:
- type of psoriasis
- extent and severity of psoriasis
- age, gender and living circumstances of the sufferer
- response of the sufferer to previous treatment
The following treatments are available for psoriasis and can also often be combined:
- local therapy: topical treatment with ointments and creams
- phototherapy: treatment with light (UVA, UVB, sometimes in combination with drugs or baths)
- conventional systemic treatment: treatment with drugs
- systemic treatment with biologics: treatment with special drugs made from or containing components of living organisms
- climate therapy: a stay in the mountains or by the sea
- complementary therapy: various topical or internal therapies
- stress management: relaxation techniques, stress management techniques, psychotherapy
- sport and exercise: for relaxation or as therapy for psoriatic arthritis.
Tips and tricks
- Apply creams regularly to avoid flare-ups.
- Use ointments, creams and lotions that are appropriate for your skin type, the climate and the season, e.g. in winter use products with a higher fat content and bath solutions containing oil. When the temperatures rise, use creams with a lower fat content.
- Keep products in the refrigerator, as refrigerated skincare products provide additional relief from itching.
- Do not use too much water and soap when washing the body.
- Protect inflamed skin areas from sun and heat, ideally by wearing loose-fitting and soft, cotton clothing.
- To reduce itching, ensure that your living accommodation is not too dry and at the right temperature; keep above 40% humidity and at a temperature between 20 and 25°C.
- Keep your fingernails short and blunt to minimise injury when scratching.
- Eat more fruit, vegetables and omega 3 food (fish, rapeseed oil) and avoid spicy food and excessive drinking.
- Feeling relaxed and at ease with oneself has a positive effect on the skin
Facts and figures
- About 2% of the global population has psoriasis.
- 95% of psoriasis sufferers have the common form of psoriasis (psoriasis vulgaris of plaque psoriasis).
Editors: aha! Swiss Allergy Centre in co-operation with the Scientific Advisory Board.



