Chronic hand eczema
Substances that are harmful to the skin, irritants, allergy-causing substances but also hereditary factors can be a reason for eczema of the hands. The symptoms differ greatly and vary in severity.

Table of contents:
Chronic hand eczema is not contagious and can persist for months or years or recur episodically. It is estimated that five to ten per cent of the total population are affected, women more commonly than men.
Causes and forms
The more frequently the skin comes into contact with irritant, harmful or allergy-causing substances and the shorter the regeneration phases between periods of contact, the more likely it is that the natural protective barriers of the skin will be exhausted.
Irritant contact hand eczema
This form of eczema is caused by external factors that irritate the skin. Constantly working in wet conditions, frequent hand washing, working with food or disinfectants, contact with oils or chemicals are the most common causal factors.
Allergic contact hand eczema
This form occurs as a result of contact with allergy-causing substances, e.g. nickel, epoxy substances, chromate, Peru balsam, fragrances.
Atopic hand eczema
A genetic predisposition to atopic dermatitis, hay fever or allergic asthma is known as atopy. People with this atopic predisposition have three times as high a risk of developing hand eczema as the average for the population because the protective barrier of their skin is often disrupted.
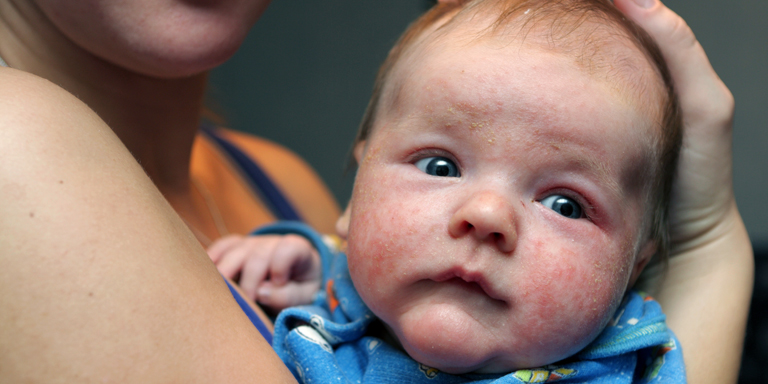
Symptoms
The symptoms differ greatly and also vary in severity:
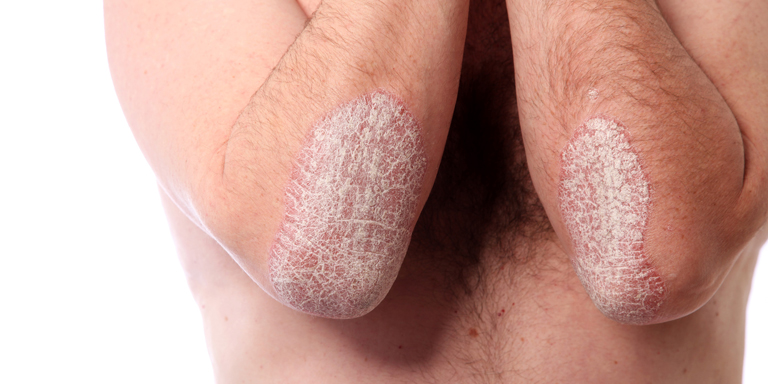
- Dry, scaling skin
- Itching
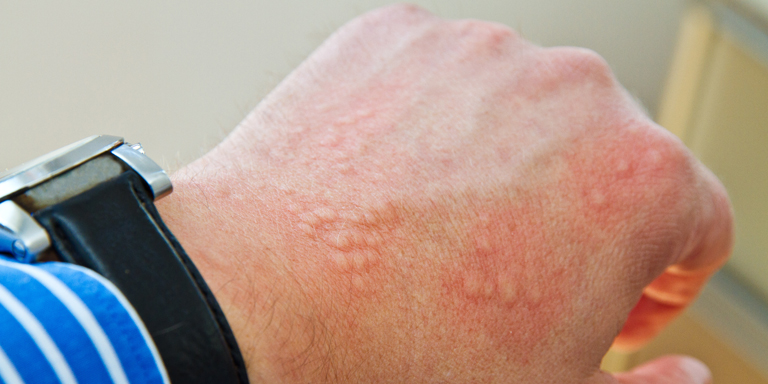
- Redness
- Splits and cracks
- Inflammation of the finger pads
- Blistering
- Impaired cornification
Diagnosis
The following questions may help identify the cause of the hand eczema:
- During which activities or during contact with which substances does the eczema improve or get worse?
- Does the condition improve during holidays?
- Were eczema, hay fever or asthma already present in childhood?
If allergic contact eczema is suspected, allergy tests by the doctor may provide information about the trigger factors.
Treatment
Skincare – the foundation
Good skincare is the foundation for all treatment. It is important to avoid triggers, i.e. irritants such as detergents or disinfectants, as well as any specific allergen. Wearing gloves with cotton glove liners can help avoid any unwanted contact.
The hands should only be washed in lukewarm water using mild, soap-free products. It is then crucial to treat the skin regularly with moisturising creams or ointments, especially after washing the hands and before any physically demanding activity. This strengthens the skin barrier and supports healing.
Medical treatment
Various treatment options are available depending on the course:
- Anti-inflammatory corticosteroid creams – for acute episodes
- Systemic corticosteroids – in severe cases, for short-term use
- Anti-itching medication – to help reduce the urge to scratch when strong
- Light therapy – for chronic or recurrent eczema
- Systemic treatment with vitamin A acid derivatives – for severe, treatment-resistant forms
- Non-corticosteroid, locally active immunomodulators – for long-term use or for sensitive skin
- Topical janus kinase inhibitors – new treatment option for inflammatory skin disease
- Systemic immunotherapies (biologicals) – for chronic hand eczema in atopic disease
- Other systemically active medication – in particularly recalcitrant cases
Early dermatological assessment is crucial to find the appropriate treatment and avoid relapses.
Tips and tricks
- Do not wash the hands too often and wash under lukewarm water.
- Use fragrance-free syndets (synthetic detergents) or hand wash oils rather than soap.
- Avoid cleaning with hand wash pastes or brushes.
- After washing, nourish the hands with moisturising creams at night and after work.
- In winter intensively moisturise the hands and wear gloves to protect against the cold.
- Avoid direct contact with cleaning agents or solvents.
- Before and during work, protect the hands against harmful substances with special skin protection creams.
- Protect the hands with gloves when working with substances that irritate the skin. Cotton gloves may also be worn under the work gloves.
- When shopping, look out for products with the Allergy Seal of Quality, these are particularly suitable for people with allergies and intolerances and are recommended by aha! Swiss Allergy Centre.
Facts and figures
Living with chronic hand eczema
The hand is an important organ of communication. Eczema sufferers can no longer take for granted entirely normal things such as "shaking hands" or simple interpersonal contact. A handshake is often painful and the reactions of others to visible and tangible skin symptoms can be upsetting. This is why eczema of the hands can be emotionally stressful, reduce self-esteem, and cause sufferers to be anxious and withdrawn. Communicating with other sufferers can help cope with eczema more easily.
A typical occupational disease
About 90 per cent of recognised occupational skin diseases are forms of contact eczema. Occupations involving activities that are stressful to the skin (e.g. hairdresser, cleaner, nursing professional or jobs in the metal or construction industry) are particularly at risk. Proper care of the skin and wearing of suitable gloves are important preventive measures.
If hand eczema is already present, we recommend consulting a dermatologist. If the eczema is occupation-induced, a notification of occupational disease should be submitted in conjunction with the employer to SUVA (Swiss National Accident Insurance Fund) or to the private accident insurance provider.
Editors: aha! Swiss Allergy Centre in co-operation with the Scientific Advisory Board.