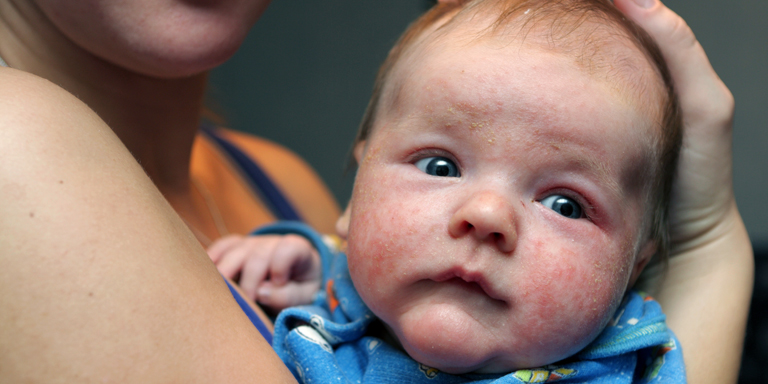
Allergic march
If in infancy and childhood one allergy form follows the next, we talk about an allergic march.
Table of contents:
The "allergic march" defines the situation where children with an allergic predisposition "grow out" of one allergic disease as they grow older, but later start to suffer from the next form of allergy. Neurodermatitis is followed by bronchial asthma and later by hay fever.
When do we talk about an allergic march?
In most cases, allergic diseases start as early as infancy and childhood and follow a characteristic pattern. Neurodermatitis (or atopic dermatitis) is followed by bronchial asthma and later by hay fever. The sequence of these three atopic diseases during childhood can be referred to as the "allergic march" (or "atopic march"). It defines the situation where children with an allergic predisposition "grow out" of one allergic disease as they grow older, but later start to suffer from the next form of allergy. All three of these conditions can co-exist or they can occur separately.
Time sequence
At the start, i.e. as early as babyhood, neurodermatitis is predominant in most cases. Up to the age of three years, 10–15% of all infants are affected by this. Over the course of months and years, most cases recover spontaneously or the itching eczema disappears completely. However, around half of the children affected go on to develop bronchial asthma, not uncommonly with symptoms as early as the second year of life. In many cases, pollen allergies are added once they reach school age.
From food to inhalation allergen
As a rule, neurodermatitis in babies occurs in connection with foods. A distinction must be made between sensitisation and allergy. A baby with a genetic predisposition may develop antibodies to foods at a very early age, mostly to hen’s eggs and milk. In this sensitisation phase, allergy symptoms will not necessarily occur. Sensitisation to foods in infancy, however, can influence the neurodermatitis and has been proved to increase the risk of later sensitisation to inhalation allergens (e.g. mites and animal hair) and the development into bronchial asthma. Thus 45% of babies sensitised to hen’s egg white later form antibodies to mites as well. 40% of them suffer from asthma by the age of five years.
Risk and early detection
The tendency to suffer from allergies as early as infancy and early childhood is directly related to the genetic predisposition, the incidence of these diseases among parents and siblings. If one parent is affected by an allergy, the risk of a child developing an allergy is around 30%. If both mother and father have allergic diseases, the risk increases to 50–70%. Questioning about the family history of allergies is currently the only way to identify at-risk children at an early stage and initiate preventive measures in a targeted way. Unfortunately, the atopic disposition in many children is not recognized until the allergic march has already begun: after eczema has first appeared or when sensitisation has been proved. This proof is obtained either by skin tests or by the identification of specific antibodies in the blood. These investigations can be done very early during infancy and early childhood. Early detection is made difficult by the fact that two-thirds of all children have no family predisposition but 15% of them nevertheless suffer from allergies during early childhood.
How can the allergic march be influenced?
There are a few generally valid recommendations for reducing the risk of sensitisation: breast-feeding during the first four to six months, a balanced diet and quitting smoking during and after pregnancy. Simple and affordable measures to reduce house dust mites in sleeping areas can also have a beneficial effect. Where babies have an atopic predisposition, it is advisable to obtain expert advice on diet. According to current wisdom, removing a house pet from the homes of families with at-risk children is no longer a top priority. The situation is different if the child has an allergy to animal hair. Allergen reduction and other preventive measures are intended to help avoid sensitisation in children with an atopic predisposition. If such sensitisation has already been detected or the first symptoms of disease have occurred, preventive and therapeutic measures should aim to limit the amount of further sensitisation and to prevent the onset of further allergies.
Author: Peter Eng MD, Specialist in Paediatric Pneumology and Allergology (Aarau and Lucerne Children’s Hospitals)
Editors: aha! Swiss Allergy Centre in co-operation with the Scientific Advisory Board.