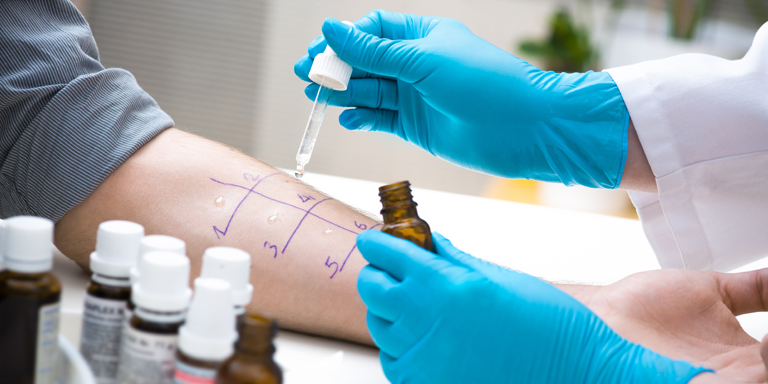
Latex allergy
Products containing latex can produce allergic reactions and even cause a cross-reaction with certain foods.
Table of contents:
Latex is the milky juice extracted from the rubber tree Hevea brasiliensis that is primarily used in the manufacture of essential medical products such as gloves and catheters but is also present in many everyday items such as balloons and earplugs. Allergic reactions usually manifest as local urticaria (hives), but sometimes also in more ominous reactions such as facial swelling, shortness of breath or shock.
Causes
Latex is used in a wide variety of products because of its physical properties, wearing comfort and low price. Different proteins in the latex can trigger allergies.
Latex items used in a medical setting
Gloves, wound drains, urinary catheters, hot water bottles, Ambu bags, blood pressure cuffs, dental wedges and rubber dams, dressings, rectal tubes, etc.
In everyday life
Balloons, condoms, erotic products, therapeutic bands, muscle strengthening bands, elastic in clothing, stretch underwear, anti-slip shower mats and bathmats, dummies (pacifiers), flip-flops, swimming caps, grips (e.g. on handbags or bicycles), hot water bottles and much more.
Powdered latex gloves more commonly trigger allergies because they have higher concentrations of latex proteins owing to different manufacturing processes. The powder can also get into the surrounding air, be inhaled and thus aggravate or even trigger symptoms.
Cross-reactions
Latex allergy sufferers may also have cross-reactions to foods in which the proteins of have a similar structure to latex allergens. These foods are typically pineapple, avocado, bananas, sweet chestnuts, figs, potatoes, kiwi-fruit, mango, melon, papaya, passion fruit, peaches, spinach and tomatoes. It is not uncommon to have a cross-allergy to a popular house plant, the weeping fig (Ficus benjamina).
Symptoms
In most cases latex allergy develops after skin or mucosa is in direct contact with materials containing latex. Direct skin contact can result in local urticaria (hives) with itching, reddening of the skin and small or large swellings. If there is no direct contact, about half of sufferers react with respiratory tract symptoms, such as asthma and allergic rhinitis, and red, itchy eyes.
Latex allergens absorbed through the skin/mucosa are spread in the body via the blood and can therefore cause urticaria (hives) anywhere on the body, swollen lips and various mucosal reactions as well as other symptoms (runny nose, asthma attacks, swelling affecting the mouth, throat and larynx, gastrointestinal symptoms). Severe anaphylactic reactions, such as a drop in blood pressure, loss of consciousness and cardiac arrest, occasionally occur.
Diagnosis
The diagnosis is based on a detailed medical history as well as skin and blood tests. Provocation tests can also be performed with items containing latex.
Treatment
People suspected of having a latex allergy should consult an allergy specialist.
Depending on the severity of the symptoms, sufferers are issued with emergency medication (antihistamine, cortisone and possibly adrenaline auto-injector) after being fully instructed on how to use them.
It is essential that anyone who has an allergic reaction to latex notify the doctors, dentists and medical staff treating them. To ensure that medical ancillary staff also act appropriately in emergencies, they should always have an allergy card with them.
Tips and tricks
- Replace items and clothes containing latex with latex-free products. Nowadays many synthetic fibres are available that can replace natural latex without loss of quality and thus minimise the risk of allergy.
- Always have your allergy card with you and ensure medical staff are aware of your allergy.
- Do not use powdered latex gloves.
Facts and figures
The incidence of latex allergy is 2% in the overall world population and 10–17% among those employed in the medical sector.
People with an atopic predisposition and those already suffering from an allergy are at higher risk of developing a latex allergy than others without these risk factors. Latex allergy is most common in the following occupational activities and sectors because of possible contact with natural latex:
- cleaning staff
- beauty and cosmetics industry
- staff working in kitchens and food companies
- medical and dental personnel (especially surgical staff)
- workers in the rubber-processing industry
- occupations involving work with seals and insulation
- anyone who has undergone multiple operations or had to undergo surgery in early childhood because of anomalies (e.g. spina bifida, kidney/bladder malformations).
Editors: aha! Swiss Allergy Centre in co-operation with the Scientific Advisory Board.