Histamine intolerance
People with histamine intolerance are unable to break down endogenous histamine and histamine supplied through diet to a sufficient extent.

Table of contents:
Histamine intolerance is thought to involve an imbalance between the supply and degradation of histamine. This imbalance gives rise to a wide variety of symptoms, which are primarily treated with a low-histamine diet. As the symptoms vary greatly, it is important to rule out other diagnoses beforehand.
Causes and trigger
Histamine is a biogenic amine. Biogenic amines are biologically active substances that perform important functions in the body, For example, they act as transmitters in allergic reactions, regulate blood pressure and have an effect on gastrointestinal movements.
The cause of histamine intolerance is not yet fully understood. It is thought that the disease arises as a result of an imbalance between the supply of histamine and reduced activity of the histamine degrading enzymes diamine oxidase (DAO) and histamine-N-methyltransferase (HNMT).
A high intake of histamine in the diet is thought to be the main cause of symptoms. Histamine is found in animal and vegetable foods in varied concentrations. Maturation and fermentation processes affect the histamine content. The fresher the food or dish, the better it is usually tolerated.
Symptoms
Histamine intolerance is a clinical picture with a wide variety of symptoms. These are frequently non-specific and mainly occur during and after meals.
Typical symptoms include:
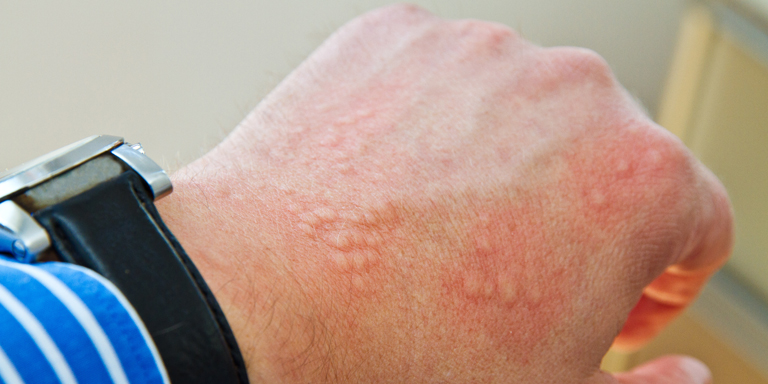
- Sudden skin redness (flush symptoms)
- Itching and redness on the body
- Digestive symptoms such as nausea, vomiting, diarrhoea, abdominal pains
- Drop in blood pressure, dizziness, palpitations
- In women: menstrual problems
- Running nose, chronic runny nose
- Headaches, migraine
- Red eyes, swollen lips
Diagnosis
Unfortunately, there are as yet no definitive tests for histamine intolerance. Blood / urine tests are often recommended to determine diamine oxidase and histamine levels in the blood. These tests have been scientifically proven to be inconclusive and are not recommended for making the diagnosis.
As the symptoms are non-specific, it is essential that food allergies and intolerances such as lactose intolerance, coeliac disease and fructose malabsorption are first excluded. Keeping a food and symptom diary can provide important insights in this regard.
If histamine intolerance is still suspected, a low-histamine diet can be tried under the supervision of a specialist dietitian. If the symptoms improve during this period, the suspicion of histamine intolerance hardens.
If there is no improvement under the low-histamine diet, then it is most likely that a histamine intolerance is not involved. In this case, the low-histamine diet should be discontinued.
Treatment
If the low-histamine diet appears to confirm or confirms the diagnosis, the next step is to determine the individual tolerance of foods containing histamine. This involves gradually increasing the amount consumed, ideally with the support of a specialist dietitian.
A strict low-histamine diet is not necessary. Where necessary, the enzyme diamine oxidase can also be taken shortly before a meal.
If the symptoms are severe, use of an antihistamine may be appropriate. However, this must be discussed with the responsible consultant.
Food overview
Histamine-rich foods
Although many food lists can be found on the internet and in books, there is little reliable scientific data available on the histamine content of foods. This is because histamine content is affected by various factors and therefore varies significantly. Moreover, the quantity of food consumed containing histamine and individual tolerance level also play a crucial role in terms of symptoms.
Foods that have undergone fermentation and maturation processes should generally be avoided. For example, anything containing alcohol, vinegar, yeast and bacteria. This includes tinned foods, convenience foods, semi-processed products, meals kept warm or reheated and products stored for a long period. The more perishable the food and the higher the protein content, the more important it is to consider freshly preparing meals.
Examples of histamine-rich foods
Meat
Any type of sausage, including fried sausage, cervelat, cold cuts, salami, air-dried beef, Mostbröckli (smoked beef), uncooked ham, ham, smoked ham, Landjäger (spicy raw sausage), etc.
Fish
Tinned, marinated, salted or dried tuna (also fresh), mackerel, sardines, anchovies, herring, seafood
Cheese
Any type of hard, soft and processed cheese (Swiss cheese contains a significantly lower quantity of histamine and is generally well tolerated)
Vegetables
Pickled cabbage, spinach, tomatoes, tomato juice, ketchup, aubergine, avocado
As well as foods that are rich in histamine, there are other foods that release histamine, such as citrus fruits, strawberries and chocolate, and cause symptoms. Other biogenic amines, such as bananas and pulses, can also cause symptoms.
Tolerable alternatives
But for a few exceptions, fresh, unprocessed food contains only small quantities of histamine and is usually well tolerated.
Examples of foods well tolerated
Meat
fresh, unprocessed or frozen meat and poultry such as thin steaks, chops, strips of meat, mince, fillet, etc.
Fish
Fresh, unprocessed or frozen fish such as cod, trout, etc.
Dairy products
Unripened cheese, e.g. cottage cheese, quark and other dairy products such as milk, yoghurt, cream, etc.
Vegetables, fruit
All types of vegetable and fruit, fresh, unprocessed or frozen.
Facts and figures
In Switzerland an estimated one per cent of the population is affected by histamine intolerance.
Editors: aha! Swiss Allergy Centre in co-operation with the Scientific Advisory Board.